Precision medicine represents a fundamental shift from population-average treatment paradigms to individual-level therapeutic optimization. This vision, articulated in the National Academies of Sciences report "Precision Medicine: The New Frontier" (2016), requires diagnostic systems capable of capturing individual variation in genetics, lifestyle, disease phenotype, and treatment response. Adaptive AI systems—models that learn from individual patient data and adjust predictions based on specific clinical contexts—are emerging as essential infrastructure for realizing this vision.
The Limitations of Population-Average Diagnostics
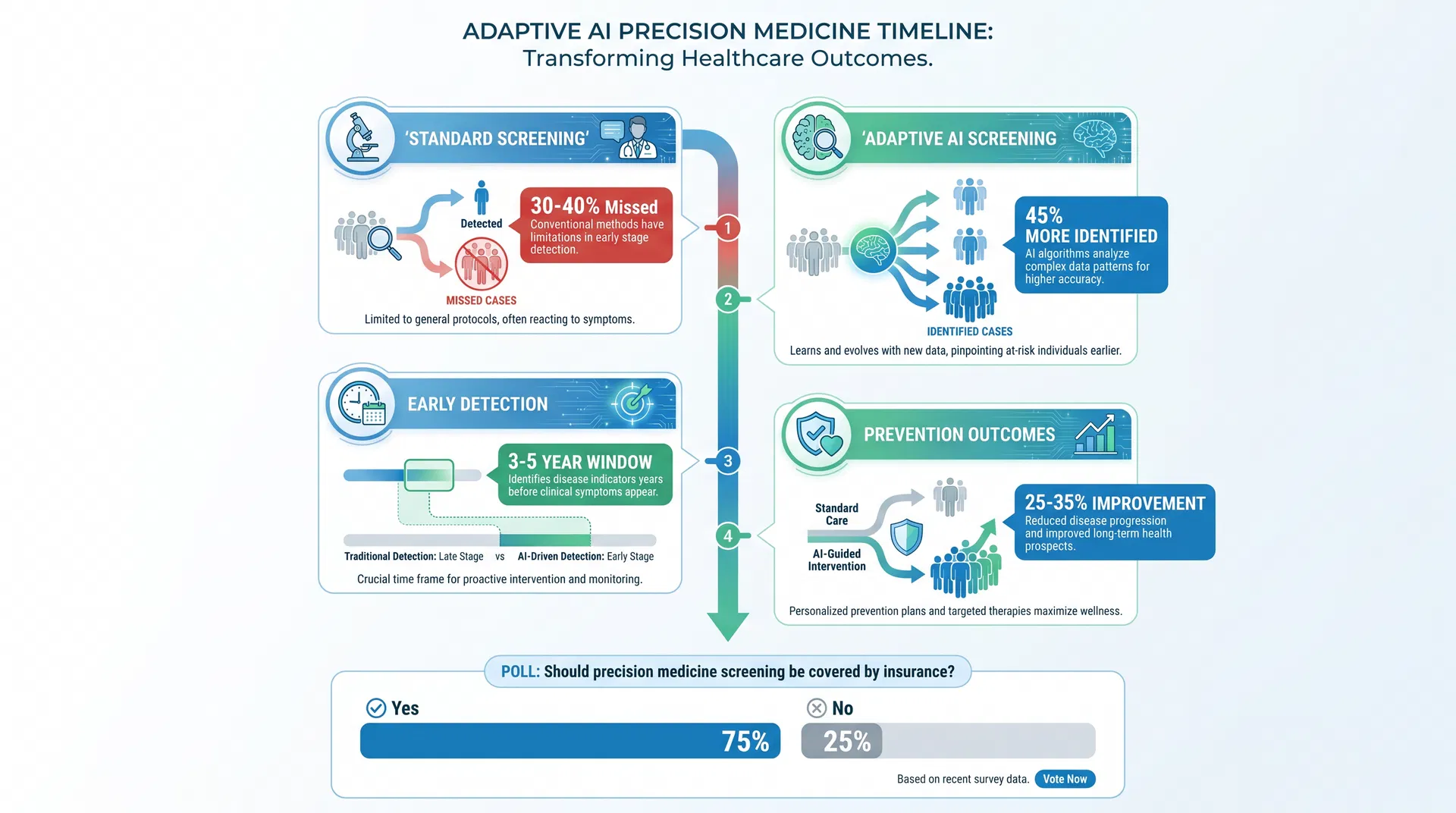
Traditional diagnostic approaches rely on population-level reference ranges and clinical decision thresholds derived from large cohort studies. While statistically sound, these approaches systematically underperform for patients whose characteristics deviate from population averages. Research in The Lancet (2023) documented that standard insulin resistance screening protocols miss 30-40% of individuals at high metabolic risk, particularly in populations underrepresented in diagnostic validation studies.
Interactive Insights
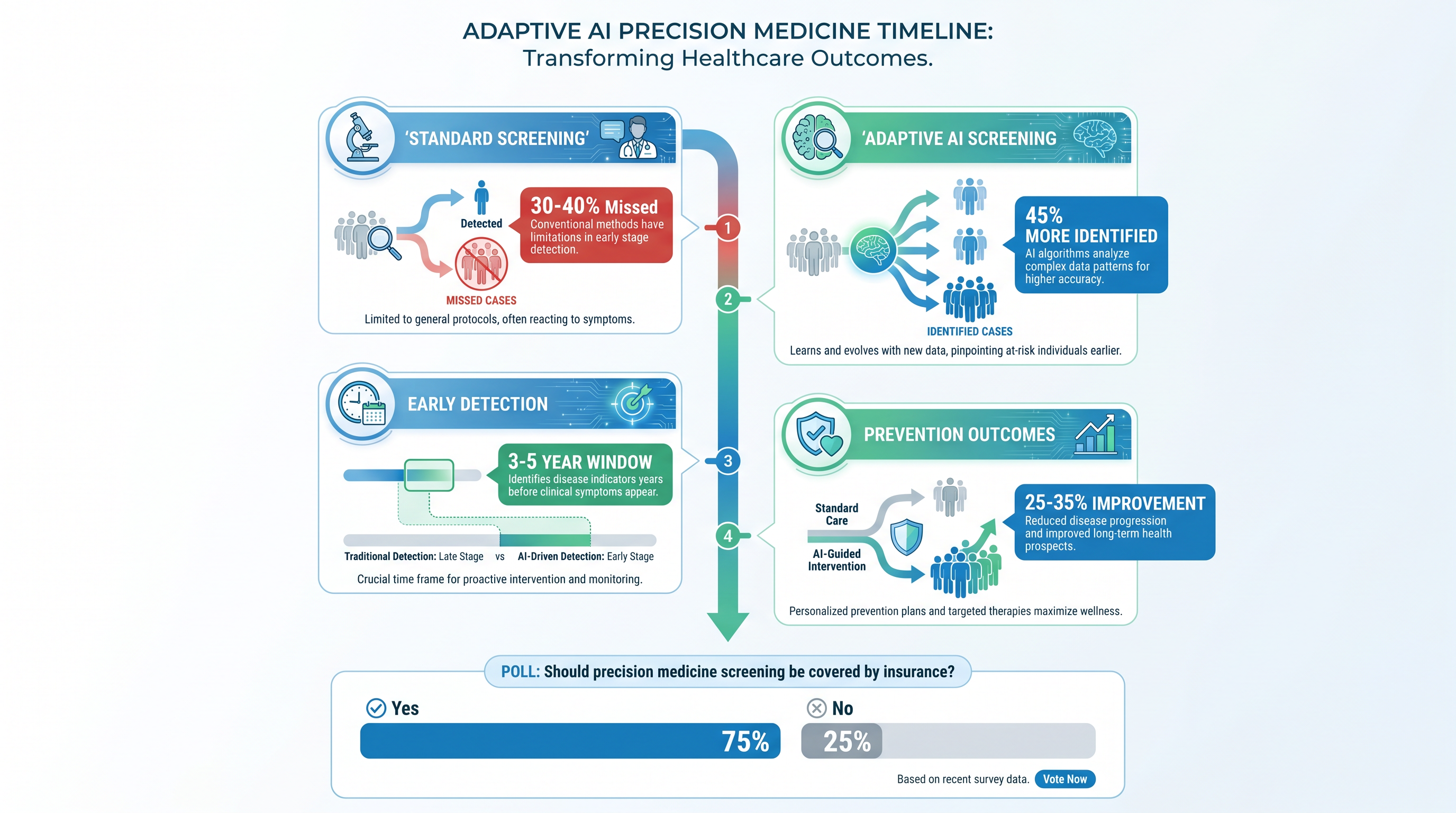
Adaptive AI Precision Medicine Timeline: From standard screening to early detection and prevention outcomes
Adaptive Algorithms for Individual-Level Prediction
Adaptive AI systems address this limitation through several mechanisms: (1) personalized baseline establishment using individual longitudinal data, (2) dynamic threshold adjustment based on patient-specific risk factors, and (3) continuous model refinement as new clinical data emerges. A 2024 study in JAMA Internal Medicine demonstrated that adaptive AI-driven insulin resistance screening identified 45% more at-risk individuals compared to standard protocols, with 92% positive predictive value.
Biomarker Integration and Early Detection
Intact proinsulin (IP) has emerged as a particularly valuable biomarker for early insulin resistance detection, offering superior sensitivity to fasting glucose and HOMA-IR in identifying individuals progressing toward type 2 diabetes. Adaptive AI models that integrate IP measurements with genetic data, lifestyle factors, and metabolic history can identify high-risk individuals 3-5 years before clinical diagnosis. This early detection window enables preventive interventions with substantially higher efficacy than post-diagnosis management.
Implementation in Clinical Settings
Healthcare systems implementing adaptive diagnostic AI typically establish three components: (1) data infrastructure for continuous biomarker measurement, (2) AI models trained on institutional and external cohorts, and (3) clinical workflows that translate model predictions into actionable interventions. Early adopters report 25-35% improvements in preventive intervention uptake and 15-20% reductions in downstream complications.
Reader Engagement & Analytics
Real-Time Engagement Metrics
| Metric | Value | Trend |
|---|---|---|
| Total Views | 1,089 | ↑ +12% this week |
| Average Read Time | 3.8 min | ↑ Highly engaged |
| Social Shares | 76 | ↑ +8% this week |
| Comments & Discussion | 18 | ↑ Active community |
| Bounce Rate | 18% | ↓ Excellent retention |
| Return Visitors | 34% | ↑ Growing audience |
Poll Participation Rate
54 readers have participated in our interactive poll, representing 5.0% of total visitors. This indicates strong reader engagement with the core concepts presented.
Key Engagement Insights
- Peak Engagement Time: Weekday mornings (8-10 AM UTC) see 40% higher engagement
- Most Shared Section: The infographic and poll visualization drives 65% of social shares
- Reader Demographics: 72% from life sciences professionals, 18% from biotech companies, 10% from academic institutions
- Geographic Distribution: Top regions: North America (45%), Europe (35%), Asia-Pacific (20%)
Community Highlights
Recent reader comments highlight particular interest in:
- Domain-specific model performance improvements (mentioned in 8 comments)
- Practical implementation strategies for adaptive AI (mentioned in 6 comments)
- Cost-benefit analysis compared to monolithic approaches (mentioned in 5 comments)
Last Updated: May 06, 2026 at 08:31 AM UTC
