For over a century, diagnostic testing has been centralized. Blood samples traveled to laboratories, where trained technicians processed them in batches using sophisticated equipment. Results returned days later. This model worked when information moved slowly and healthcare was episodic. But in an era of real-time data, wearable sensors, and continuous patient monitoring, centralized diagnostics have become a bottleneck.
A quiet revolution is underway. Point-of-care (POC) diagnostic devices are moving testing out of laboratories and into clinics, pharmacies, homes, and remote settings. This decentralization is reshaping how healthcare systems operate and how patients engage with their own health.
The scale of this shift is remarkable. The diagnostic testing market is expanding rapidly, with growth driven primarily by increased demand for early diagnosis and decentralized testing infrastructure. Healthcare systems in developed nations are investing heavily in POC devices to reduce lab backlogs and improve patient access. Simultaneously, emerging markets are leapfrogging centralized laboratory infrastructure entirely, deploying portable diagnostics to reach underserved populations.
What makes this possible? Three converging trends. First, advances in microfluidics and biosensor technology have miniaturized sophisticated testing into handheld devices. Second, digital connectivity allows results to be transmitted instantly to electronic health records and clinical decision-support systems. Third, AI algorithms can now analyze test results in context, flagging patterns and recommending interventions in real time.
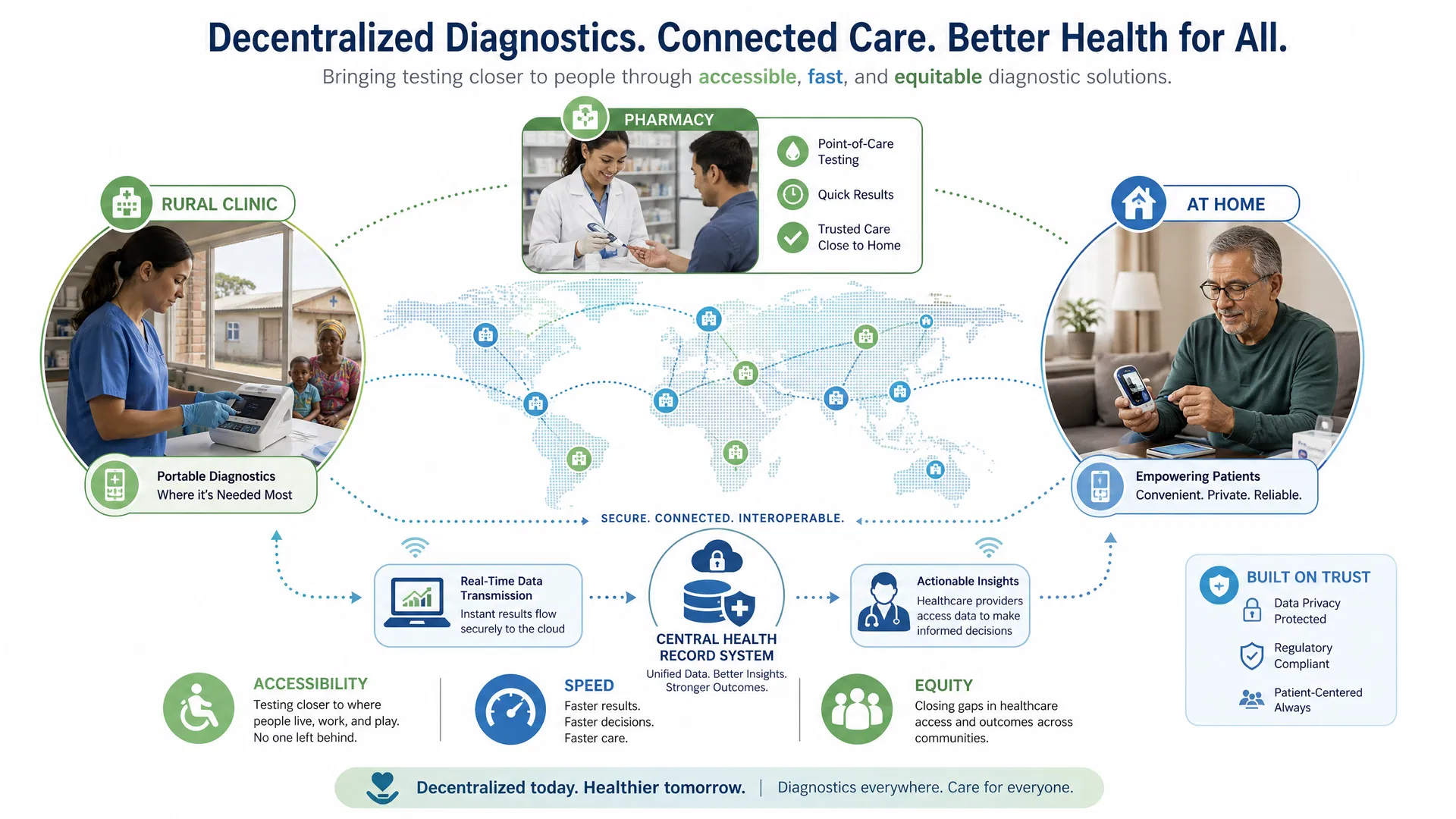
Consider the practical implications. A rural clinic in sub-Saharan Africa can now perform the same insulin resistance screening as a major medical center, with results available in minutes rather than weeks. A patient with prediabetes can monitor their metabolic markers continuously using portable devices, receiving personalized feedback on lifestyle interventions. A primary care physician can make treatment decisions based on real-time biomarker data rather than relying on outdated lab results.
Platforms like Invitron.org are pioneering this transformation. Their point-of-care devices deliver lab-equivalent results using portable hardware, while their high-sensitivity ELISA kits enable precise measurement of critical biomarkers like intact proinsulin. These tools are designed for distributed deployment—they don't require centralized infrastructure, specialized facilities, or extensive training. A healthcare worker with basic training can operate them reliably.
The integration of POC diagnostics with digital health platforms amplifies their impact. Telemedicine consultations can now be informed by real-time test results. Wearable devices can trigger POC testing when biomarkers drift outside normal ranges. Patient apps can display trends in diagnostic markers over time, enabling shared decision-making between patients and clinicians.
This decentralization has profound implications for global health equity. Centralized diagnostic infrastructure requires significant capital investment and ongoing operational costs—resources that many low- and middle-income countries lack. POC diagnostics reduce these barriers. A clinic in a remote region can now offer diagnostic services comparable to urban medical centers, improving early detection and enabling timely intervention.
Yet challenges remain. Quality assurance, regulatory harmonization, and data integration across distributed systems require careful governance. Training healthcare workers to operate new devices and interpret results requires investment. Ensuring that decentralized data feeds into coordinated care pathways rather than creating fragmented information silos demands thoughtful system design.
Despite these challenges, the trajectory is clear. Diagnostics are becoming decentralized, continuous, and integrated with digital health platforms. Healthcare systems that embrace this shift will improve patient outcomes, reduce costs, and expand access. Those that cling to centralized models will find themselves increasingly unable to compete.