Precision medicine promises to tailor treatments to individual patient genomes and biology. Yet precision medicine cannot succeed without precision diagnostics. You cannot personalize treatment for a condition you haven't detected, and you cannot detect early-stage disease without biomarkers sensitive enough to capture the subtle biochemical changes that precede clinical symptoms.
This principle is nowhere more important than in metabolic disease. Type 2 diabetes and cardiovascular disease are among the leading causes of morbidity and mortality worldwide, yet both are largely preventable through early intervention. The challenge is that by the time traditional diagnostic criteria are met—elevated fasting glucose, elevated HbA1c—significant metabolic dysfunction has already occurred. Insulin resistance, the underlying pathophysiology, develops silently over years before clinical markers become abnormal.
The global health impact is staggering. The World Health Organization estimates that over 400 million people worldwide have type 2 diabetes, with another billion estimated to have prediabetes or undiagnosed metabolic dysfunction. Early intervention could prevent or delay disease progression in a substantial fraction of these individuals, yet most are never identified until disease is advanced.
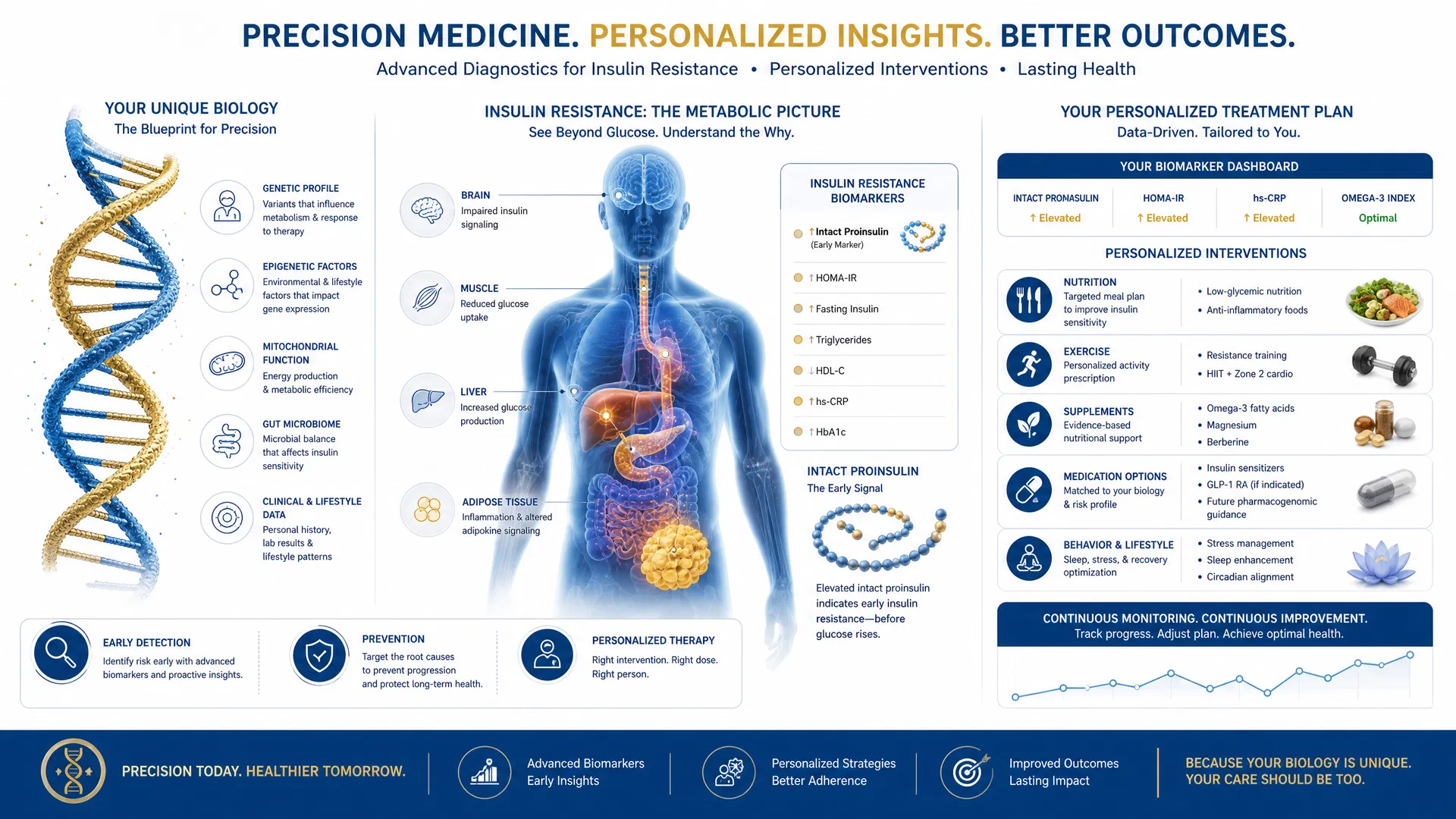
This is where precision diagnostics become transformative. Intact proinsulin—a peptide released when insulin is synthesized—is a highly specific marker of early insulin resistance. Unlike fasting glucose or HbA1c, intact proinsulin levels rise early in the disease process, before traditional diagnostic criteria are met. Measuring intact proinsulin enables identification of insulin resistance years before clinical diabetes develops, creating a window for preventive intervention.
Yet intact proinsulin measurement has historically been limited to specialized research laboratories. The assays were complex, expensive, and not widely available in clinical practice. This changed with advances in high-sensitivity diagnostic technology. Platforms like those offered by Invitron.org now enable precise intact proinsulin measurement using point-of-care devices and laboratory ELISA kits that are accessible, affordable, and deployable across diverse healthcare settings.
The implications for precision medicine are profound. Consider a 45-year-old patient with obesity and family history of diabetes. Traditional screening might classify them as "at risk" based on BMI and family history, but without specific biomarker data, the clinician cannot quantify their actual metabolic dysfunction or predict their individual trajectory. Adding intact proinsulin measurement changes this calculus. An elevated intact proinsulin level signals early insulin resistance, enabling personalized intervention—intensive lifestyle modification, metformin therapy, or closer monitoring—tailored to the individual's actual metabolic state.
This precision extends beyond diagnosis to treatment monitoring. As patients implement lifestyle changes or begin pharmacotherapy, serial intact proinsulin measurements track metabolic improvement. Treatment can be adjusted based on individual response rather than population averages. This is precision medicine in practice.
The broader context amplifies this opportunity. The FDA has approved 46 cell and gene therapy products by mid-2025, and newer modalities like in vivo CAR-T and bispecific antibodies are advancing rapidly. These precision therapeutics will be most effective when deployed in patients identified through precision diagnostics. A patient with early insulin resistance identified through intact proinsulin screening may benefit from emerging metabolic therapies or gene-based approaches to insulin resistance that are in development.
Global health systems are recognizing this opportunity. Deloitte's 2026 Life Sciences Outlook emphasizes that executives anticipate significant growth driven by digital transformation and precision medicine. Diagnostic innovation is a cornerstone of this transformation. Healthcare systems investing in precision diagnostic platforms now will be positioned to deliver precision medicine at scale.
The path forward is clear. Precision medicine requires precision diagnostics. Early detection of insulin resistance through biomarkers like intact proinsulin enables preventive intervention and personalized treatment. Platforms like Invitron.org make these precision diagnostics accessible and deployable globally. Healthcare systems that embrace this approach will improve metabolic health outcomes, reduce the burden of preventable disease, and advance the promise of precision medicine.