The Sewer as Sentinel: How Wastewater Surveillance Is Transforming Pathogen Detection and Public Health Early Warning
The Invisible River of Public Health Intelligence
Every day, billions of people contribute to one of the most comprehensive and underutilised public health surveillance systems in existence: the municipal wastewater network. When a person is infected with a pathogen — whether they develop symptoms or not — they shed viral particles, bacterial cells, and genetic material into their bodily waste. That waste flows through sewers, converges at wastewater treatment plants, and in doing so, creates a pooled, population-level biological sample that reflects the infectious disease burden of an entire community.
Wastewater surveillance, also known as wastewater-based epidemiology (WBE), is the systematic analysis of this pooled sample to detect, quantify, and track pathogens circulating in a community. It is, in the most literal sense, a sentinel system: a continuous, passive, and population-wide monitor that can detect the presence of a pathogen in a community before clinical cases begin to appear in hospitals and testing laboratories.
The COVID-19 pandemic transformed wastewater surveillance from a niche research methodology into a mainstream public health tool. The discovery that SARS-CoV-2 RNA could be detected in wastewater days to weeks before clinical case counts began to rise demonstrated the extraordinary potential of this approach as an early warning system — and catalysed a global expansion of wastewater surveillance infrastructure that continues to this day.
The Science of Wastewater Surveillance
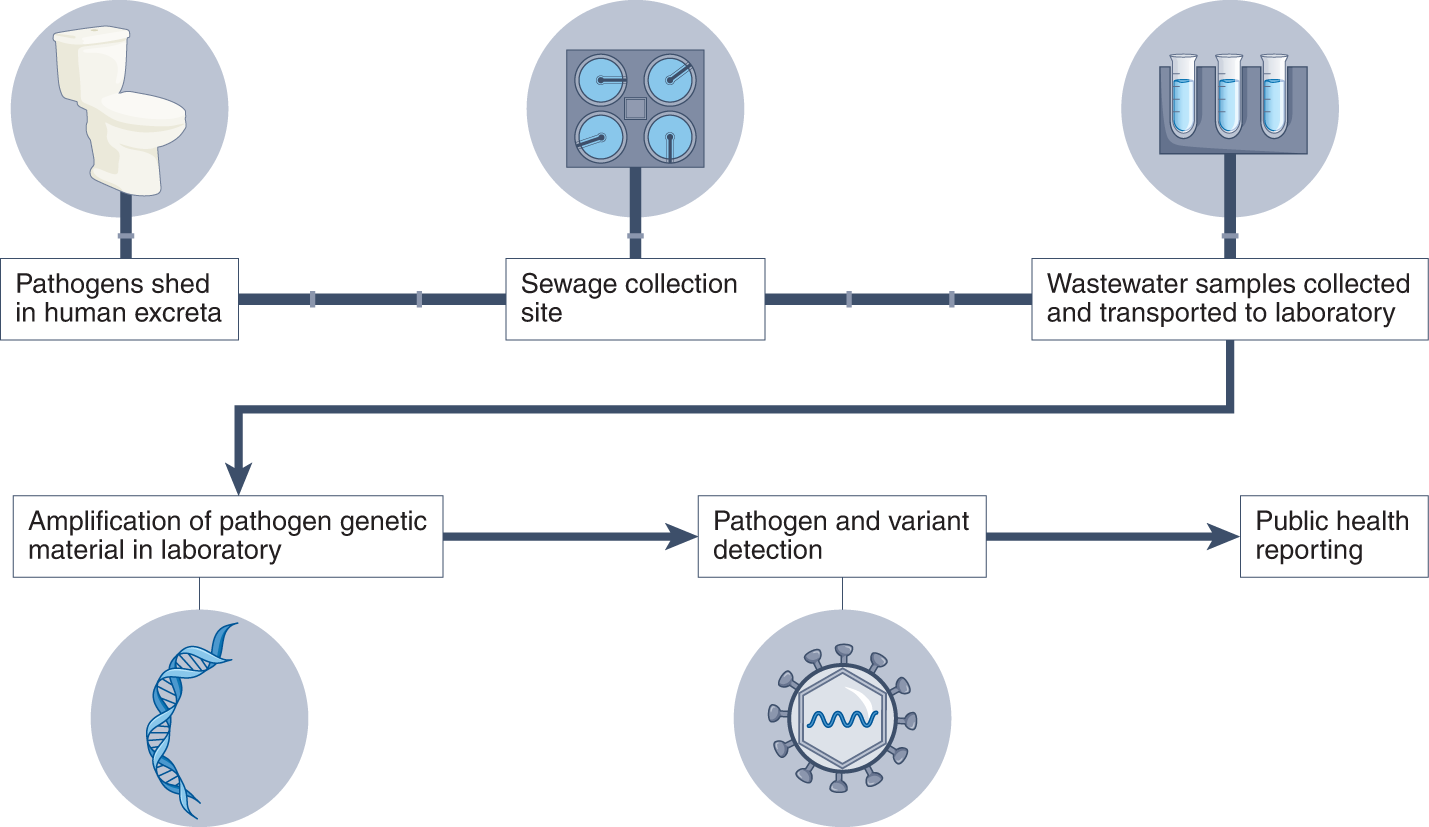
The fundamental principle of wastewater surveillance is straightforward: pathogens shed by infected individuals in a catchment area accumulate in the wastewater flowing to a treatment plant, where they can be collected, concentrated, and analysed using molecular techniques.
The workflow typically proceeds through five stages:
| Stage | Process | Key Considerations |
|---|---|---|
| Sample Collection | Composite or grab samples collected from wastewater treatment plant influent or sewer network nodes | Timing, flow-weighted sampling, temperature stability |
| Concentration | Viral particles or nucleic acids concentrated from large water volumes | Ultrafiltration, polyethylene glycol precipitation, electronegative membrane filtration |
| Nucleic Acid Extraction | RNA or DNA extracted from concentrated sample | Inhibitor removal, extraction efficiency |
| Detection and Quantification | RT-qPCR, ddPCR, or metagenomic sequencing used to detect and quantify target pathogens | Sensitivity, specificity, multiplexing capacity |
| Epidemiological Interpretation | Signal normalised to population size and wastewater flow; trends correlated with clinical data | Normalisation biomarkers (PMMoV, crAssphage), catchment population estimation |
The sensitivity of wastewater surveillance is remarkable. Studies conducted during the COVID-19 pandemic demonstrated that SARS-CoV-2 RNA could be detected in wastewater when as few as one in 100,000 to one in 1,000,000 community members was infected — a sensitivity that far exceeds what clinical testing can achieve, particularly in settings where testing rates are low or asymptomatic cases are common.
Why Wastewater Surveillance Outperforms Clinical Surveillance
Clinical surveillance — the monitoring of confirmed cases through healthcare systems and testing laboratories — is the backbone of infectious disease epidemiology. But it has fundamental limitations that wastewater surveillance is uniquely positioned to address.
Clinical surveillance is biased towards symptomatic cases. The majority of individuals infected with many pathogens — including SARS-CoV-2, poliovirus, and norovirus — either develop no symptoms or develop symptoms too mild to prompt healthcare-seeking behaviour. These asymptomatic and mildly symptomatic individuals are largely invisible to clinical surveillance systems, yet they may contribute substantially to community transmission.
Clinical surveillance is subject to testing behaviour. The number of confirmed cases reported by a clinical surveillance system reflects not only the true prevalence of infection but also the rate at which people seek testing, the availability of testing infrastructure, and the sensitivity of the tests being used. During the COVID-19 pandemic, confirmed case counts varied enormously across countries and time periods in ways that reflected testing policy as much as true disease burden.
Clinical surveillance lags behind actual transmission. From the time of infection to the time a case is confirmed and reported, several days to weeks typically elapse — time during which transmission continues undetected. Wastewater surveillance, by contrast, can detect rising pathogen concentrations in the community before the first clinical cases are reported, providing the critical lead time needed to mount an effective public health response.
The COVID-19 Proof of Concept
The COVID-19 pandemic provided the most extensive and rigorous validation of wastewater surveillance as a public health tool in history. Across dozens of countries, wastewater surveillance systems consistently detected rising SARS-CoV-2 concentrations 4 to 7 days before corresponding increases in clinical case counts — a lead time that, if acted upon, could have enabled earlier implementation of control measures and potentially prevented thousands of deaths.
The United States Centers for Disease Control and Prevention (CDC) established the National Wastewater Surveillance System (NWSS) in September 2020, which grew to cover hundreds of sites serving tens of millions of people. The system demonstrated not only the ability to detect rising case counts but also to track the emergence and spread of new variants — including Delta and Omicron — before they were detected through clinical sequencing programmes.
Beyond SARS-CoV-2, the COVID-19 experience catalysed the expansion of wastewater surveillance to a much broader portfolio of pathogens, including influenza, respiratory syncytial virus (RSV), mpox, poliovirus, and antimicrobial-resistant bacteria. The infrastructure built for COVID-19 surveillance is now being repurposed as a general-purpose early warning system for infectious disease threats of all kinds.
Wastewater Surveillance and Biosecurity
From a biosecurity perspective, wastewater surveillance represents a particularly valuable capability. Unlike clinical surveillance, which depends on infected individuals seeking healthcare, wastewater surveillance is passive and continuous — it does not require any action on the part of the infected individual or the healthcare system to generate a signal. This makes it highly resistant to the kind of surveillance gaps that can allow a biological threat to spread undetected.
For biosecurity applications, wastewater surveillance can serve as an early warning system for the deliberate release of biological agents in an urban environment. A sudden, unexplained spike in a pathogen signal at a wastewater treatment plant — particularly one that does not correspond to any known seasonal pattern or clinical case cluster — could provide the first indication of a biological incident, enabling a rapid response before widespread exposure occurs.
The integration of wastewater surveillance with AI-powered anomaly detection and genomic sequencing creates a biosurveillance system of extraordinary sensitivity and specificity — one that can detect novel or engineered pathogens as well as known ones, and that can provide real-time intelligence about the geographic distribution and temporal dynamics of any biological threat.
References
- CDC National Wastewater Surveillance System — Overview of the US national wastewater surveillance infrastructure. Available at: https://www.cdc.gov/nwss/about.html
- Diamond et al. (2022) — "Wastewater surveillance of pathogens can inform public health responses." Nature Medicine. Available at: https://www.nature.com/articles/s41591-022-01940-x
- RAND Corporation (2023) — "Testing the Waters: Using Wastewater Surveillance as an Early Warning System." Available at: https://www.rand.org/pubs/commentary/2023/12/testing-the-waters-using-wastewater-surveillance-as.html